Going to bed with a herniated disc can be one of the hardest things to do in life. The feeling of pain each time you shift the body slightly means finding the right position to lie down can seem impossible.
Even when you do figure out a specific position that offers comfort, the probability of waking up in another at some point in the night is high. This means while you may go to bed pain-free, shifting positions can lead to some discomfort.
Sleeping After Herniated Disc Surgery
Have you just undergone herniated disc surgery or booked for one in a few days? One of your most dreadful thoughts is probably how you’re going to sleep after the procedure.
However, most people sleep just fine in their regular positions after undergoing this sort of surgery. To be sure, discuss sleeping options with the surgeon before and after the procedure. This way, you can avoid any positions that may increase your pain.
How do you Sleep with Herniated Discs?
The tips below can help lower the pain and discomfort when you’re suffering from a herniated disc. As long as you’re mindful of them, you could have a relatively good night.
- Proper Alignment: Remember, whatever position you choose, the correct alignment of the spine is critical. Make sure it is aligned properly with other body parts such as the neck, shoulders, and hips.
- Precautions during movement: Try to move your whole body together instead of twisting and turning certain parts at each opportunity. During movements, make sure your core is kept tight and pulled in
- Pillows, pillows, and more pillows: Do not hesitate to use pillows to provide more comfort as and when you need it. As noted above, a pillow or two can come in handy in almost any sleeping position. While pillows may provide lots of support for the neck, make sure to incorporate body pillows as well. These can be used to prop up areas such as the knees and abdomen to relieve the pressure on the spine depending on your sleeping position of choice.
- Good Mattress: If your current mattress is showing signs of wear and tear, sleeping can become even more difficult. The last thing your spine needs is a sleeping surface that makes it impossible to achieve the flat neutral position the body prefers.
- Proper posturing: Proper posturing may lower the risk of suffering a slipped disc. Avoid walking with a slouch and always try to sit upright in chairs that offer quality support. Also, if the nature of your job demands continuous sitting for hours, try to take breaks every 1-2 hours.
- Light Yoga: Yoga poses may seem next to impossible when you’ve just been diagnosed with a herniated disc. But, several light poses can be incorporated into your life without problems. Undertaking these poses may help strengthen the core and undo some of the disc degeneration caused by the natural aging process.
Precautions To Take In Bed When You’re Suffering from a Herniated Disc
As you already know by now, herniated discs can make sleeping very difficult. Finding the right position could be critical to prevent aggravation of the pain and discomfort. Here are additional tasks you should avoid while lying down in bed.
- Tossing and turning unnecessarily
- Lifting heavy stuff such as toddlers
- Switching between different sleeping positions
- Discarding the support from pillows
- Getting up from the bed suddenly
Best Sleeping Positions For Herniated Discs
OK, so you’ve been diagnosed with herniated discs. The condition can certainly make sleeping difficult. However, as long as you choose the right sleeping position, pulling through the night unscathed should be possible.
Here are the best positions for enjoying nighttime rest with a herniated disc:
1. Sleep On The Side With Knee Pillow
Lying down on the side with a pillow nudged between the knees is one of the best ways to sleep with herniated discs. We recommend this position when back sleeping hurts especially since the side position reduces the pressure on the spine.
The presence of a pillow between the knees can create proper alignment for the spine, pelvis, and hips. However, avoid lying down on one side throughout the night unless switching to the other side aggravates the pain. You wouldn’t want to suffer muscle imbalance or scoliosis down the line, would you?
Additionally, depending on your comfort needs, you may either choose one or two pillows for placement between the knees.
I love resting my knees on the ComfiLife Orthopedic Knee Pillow from Amazon. It provides maximum support and comfort throughout the night. No wonder it is the number-one-rated model on Amazon with over 11 000 5-star reviews and counting.
2. Fetal Position
This position can provide soothing relief from slipped discs. Named after the position of a baby in a women’s uterus, it involves sleeping on the side but in a curled angle. This is a great position because curling the torso opens up the space between the vertebrae which eases the pressure on the spine caused by the disc protrusions.
The result is a significant lowering of the symptoms and enhanced comfort by the time you wake up in the morning.
3. Sleeping On The Tummy With A Pillow Under The Abdomen
If you’re a dedicated stomach sleeper, lying down on the tummy with a pillow under the abdomen can be a comfy way of resting at night. Well, you may have heard that stomach sleeping is a big no-no for herniated discs and other forms of back pain.
While there may be some truth to that, placing a pillow under the abdomen can shore up support for the back and relieve some of the stress from the spinal region. Healthline says this may be the best position for herniated discs thanks to the ability to soothe the discomfort emanating from the space between the vertebrae.
4. Back Sleeping With A Pillow Under the Knees
Lying down on the back can feel daunting when you’re experiencing significant pain due to disc herniation. However, some people say this is the most comfortable position to sleep when suffering from the condition.
The trick is to keep the spine in a neutral position by placing a pillow under the knees while lying on the back.
Remember, back sleeping promotes even weight distribution on the body. This eliminates a significant chunk of pressure points resulting in a superior alignment of the spine with the critical body organs.
5. Sleeping In A Reclined Position
Do you have a recliner or adjustable bed at home? It could come in handy if you prefer lying down in a reclined position. Adjustable beds, in particular, may offer world-class alignment to prevent aggravation of the slipped discs and more pain in the morning.
Sleeping on the back in a reclined position can create an angle between the thighs and back. This angle may help lower the pressure on the back meaning a better night’s rest regardless of how severe your condition might feel.
The JUMICCO Fabric Recliner Chair from Amazon felt life-saving while I recovered from herniated disc surgery. It features breathable fabric with thick padding for the ultimate comfort throughout the night. It also sports an armrest and footrest for elevating the legs.
What Is A Herniated Disc?
Spinal pain is very common in the adult population. With 50 percent of working Americans reporting signs of back pain in the morning, the situation is quite dire.
According to the Mayo Clinic, the most common causes of back pain include:
- Herniated discs
- Bulging discs
- Muscle or ligament strain
- Arthritis
- Skeletal Irregularities
- Osteoporosis
It is important to understand what a herniated disc is. Shall we take a look at what the condition entails?
A herniated disc occurs when there’s a problem with the rubbery cushions known as discs located between the independent bones that add up to form the vertebrae to protect the spine.
Each spinal disc is made up of 2 parts i.e. nucleus and annulus. The nucleus features a soft jelly-like material that is protected by the hardy, rubber-like exterior known as the annulus. A herniated disc occurs when there’s a tear in the annulus which causes a section of the nucleus to push through it.
How Do Herniated Discs Occur?
We’ve discussed the science behind herniated discs but how do they occur in real-life? Well, herniated discs may be caused by 3 main scenarios. Let us take a closer look at each of them.
1. Spinal Degeneration
Unfortunately, anyone can suffer a herniated disc particular as you grow older. As the aging process goes on, the discs begin to lose their flexibility meaning the least twists can result in herniation.
Remember, one of the main responsibilities of the back region is to support and redistribute the body’s weight. The discs offer support from shocks as we twist, turn, and undertake activities that would otherwise strain the back.
Since these discs are constantly in use as we go about our normal daily routines, suffering wear and tear over time becomes inevitable. Thus, the nucleus can penetrate the annulus when the latter becomes weaker, leading to herniation of one or more discs.
2. Sudden Injury or Extensive Shocks
Sudden injuries such as car accidents or falls can cause enough trauma to the discs in your spine, leading to herniation. Using extensive force during physical activity such as powerlifting may also cause the discs to herniate if there are any errors in your technique.
3. Physical Trauma and Spinal Regeneration
A combination of physical trauma from an injury or sudden twist or bending coupled with spinal degeneration can cause the discs to herniate. Keep in mind that regardless of who you may be, the aging process takes a significant physical toll on the body eventually.
Things or tasks you could complete without stress in the past may cause sudden injury now thanks to spinal degeneration.
There have even been instances of people suffering herniated disc incidents from activities as simple as sneezing among those with extensively weakened spinal areas.
Where Do Herniated Discs Occur?
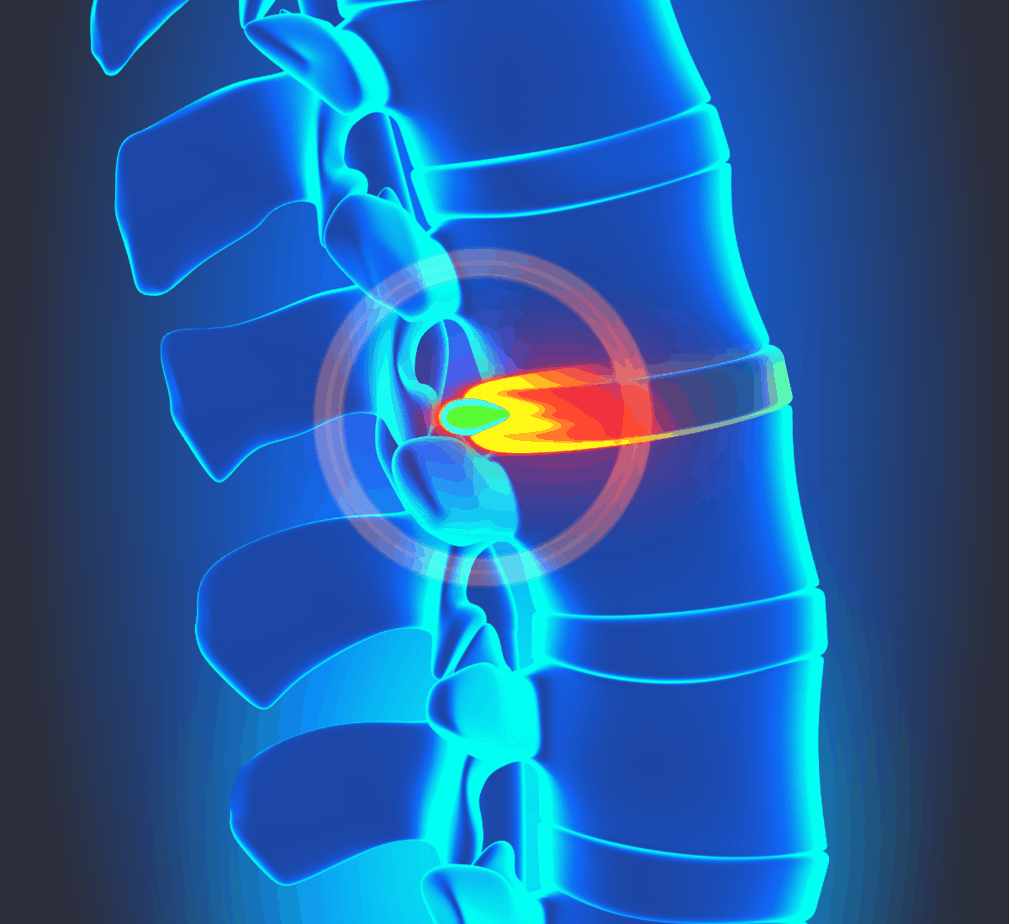
The lower back is probably the most active portion of the spinal region in a physically active person’s life. From lifting to running and other workouts, this part of the spinal region may undergo significant levels of stress during physically strenuous activities.
No wonder herniated discs normally occur in the lower back. Also, jobs that force people to sit in the same spot for hours such as airline pilots and truck drivers may lead to a greater chance of suffering a disc herniation.
The cervical spine area can also be prone to slipped discs. It may cause a lot of pain in the neck region which can even extend to the shoulders and arms. Besides, a herniated disc in the neck could even affect the ability to use the arm fully.
The discs in the mid-to-upper part of the back, known as the thoracic spine, can also be prone to herniation. When that happens, the pain and discomfort may radiate from the thoracic spine to the upper back, shoulders, and hands. It can also radiate downwards to the lower back, buttocks, and even thighs.
What Are The Symptoms of Herniated Discs?
The symptoms of herniated discs can vary from person to person, depending on the site of the herniation and other factors. Since age is an underlying reason behind spinal degeneration, it is only normal that herniation in older adults and senior citizens is relatively more severe.
The signs of herniated discs may include:
- No Symptoms: A majority of people experience no signs from slipped discs and since the condition typically heals on its own, you might experience it without even noticing any physical trauma.
- Pain: This is the obvious sign that your discs may have slipped in a particular spot. For instance, you can expect a significant degree of lower back pain after suffering a herniation in that area of the spine. Walking, standing, or sitting may become extremely painful.
- Tingling or Numbness: If you’re feeling a sudden degree of numbness or tingling in any part of the back region, chances are you may be suffering from a herniated disc. This is especially common among those who sit continuously for hours due to the nature of their job. Once you notice signs of tingling, it is time to book an appointment with your doctor.
- Muscle Weakness: Muscle weakness is another common sign of herniated discs. It can be so severe that the muscles in the affected area may feel useless.
- Severe Nerve Damage: Untreated cases of herniated discs can lead to permanent nerve damage in the long-term. In rare instances, slipped discs may affect the lower back and legs to the point where you could lose bladder and bowel control.
- Saddle Anesthesia: Nerve compression as a result of the herniated discs can make you lose sensation in the thighs, rear of the legs, and rectal muscles.
Treatments for Herniated Discs
There are multiple courses of treatments for slipped or herniated discs. A few of the most popular options available include:
1. Time
The saying that “time heals wounds” rings true for herniated discs. In most cases, you only have to give yourself enough time to heal completely.
During that period, staying away from physical activities that can affect the back such as lifting heavy objects, undertaking strenuous exercises, or remaining seated at one spot continuously for hours may be rewarding.
There have been many instances of people healing completely from the condition just by waiting it out.
2. Medications
If the feeling of pain, numbness, or tingling seems unbearable, it is time to speak to your doctor. There are several prescription drugs commonly recommended for treating the pain associated with herniated discs. If booking a doctor’s appointment takes time, over-the-counter anti-inflammatories such as ibuprofen or aspirin could come in handy.
3. Cortisone Injections
Oral medication treatments should alleviate the pain and discomfort associated with herniated discs. However, if you’re still experiencing those symptoms without any signs of improvement, your doctor may prescribe cortisone injections.
These are cortisone-based steroids injected into affected areas to provide relief. Most professionals rely on spinal imaging to administer these injections to guarantee the right results.
3. Ice/Heat Treatments
Cryotherapy, commonly known as cold treatments can be a valuable tool for herniated disc patients. Most people report gaining relief from the numbness and pain after applying ice packs on the affected area for about 20-30 minutes.
Heat therapy can also be another potent solution for slipped discs treatments. Heating pads and heat-based electronic massagers are known for providing soothing relief for patients.
4. Physical Therapy
Depending on the extent of the injury and the affected area, your doctor may prescribe physical therapy. The good news is that the majority of chiropractors and physical therapists have lots of experience treating patients with these symptoms.
Coming up with a treatment plan that improves the pain and discomfort without aggravating the current condition is what they do.
5. Surgery
Surgery may be the last resort for treating herniated discs when all of the above-named treatment options fail to improve the condition. Mayo Clinic says your doctor will only contemplate surgery when you’ve experienced little to no relief after 6 continuous weeks of treatment.
Surgery to remove a portion of the ruptured disc to provide relief for your symptoms is quite popular. Risk factors that may influence a doctor to resort to surgery may include:
- Significant pain
- Significant tingling and numbness
- Walking or standing difficulties
Conclusion
Congratulations on reading this guide for sleeping with a herniated disc. We’ve shared practical steps that can help improve the quality of your sleep despite how much discomfort you may be suffering.
While many cases of herniated discs heal on their own, try to seek medical attention as early as possible. Always check in with your doctor regularly to give an update of the pain as well as any problems you may be experiencing.
